You’ve probably felt it — that stomach drop when you get bad news, the nausea before something terrifying, the way your gut seems to physically respond to your emotional state before your mind has even fully processed it. That’s not coincidence. That’s biology. The relationship between stress and gut health is one of the most well-documented and most underappreciated connections in medicine.

Stress and Gut Health: Understanding the Gut-Brain Axis
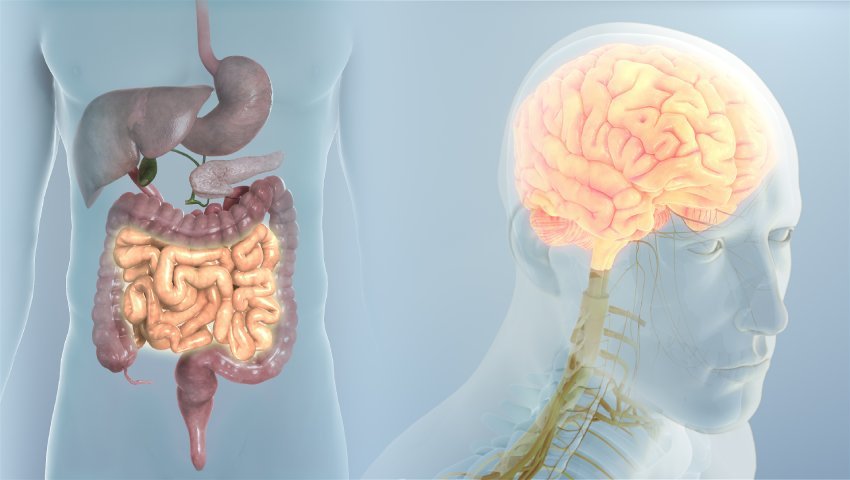
Stress and gut health are connected through the gut-brain axis, a communication network between the brain and digestive system that directly influences digestion and emotions.
There’s an actual physical communication highway between the gut and the brain. The enteric nervous system — sometimes called the ‘second brain’ — lines the gastrointestinal tract and contains roughly 500 million neurons. It communicates constantly with the central nervous system via the vagus nerve and an exchange of neurotransmitters. Serotonin? About 95% of it is produced in the gut. This system doesn’t just respond to stress — it participates in creating the stress response.
What Stress Does to Your Digestive System
Stress and gut health interactions affect digestion by altering gut movement, increasing acid production, and reducing nutrient absorption.
When you’re stressed, your body activates the fight-or-flight response. Blood flow is redirected away from the digestive system toward the muscles and heart. Digestive motility changes — sometimes speeding up (diarrhea), sometimes slowing down (constipation). Stomach acid production can spike. The gut becomes more permeable — what’s sometimes called ‘leaky gut’ — allowing bacteria and inflammatory compounds to cross into the bloodstream. The microbiome itself shifts. Beneficial bacteria can decrease. Inflammatory species can proliferate.
None of this happens dramatically in a single stressful moment. But chronic, sustained stress — the kind that’s become background noise in modern life — creates cumulative changes that genuinely alter gut function.
Stress-Related Gut Symptoms
Stress and gut health problems can cause symptoms such as bloating, nausea, constipation, diarrhea, and acid reflux.
The list of what stress and gut health disruption can produce is long:
- Nausea that appears before or during stressful events
- Urgency to use the bathroom — the gut speeding up under sympathetic activation
- Constipation in people who tend toward a freeze response rather than flight
- Heartburn and acid reflux, because the lower esophageal sphincter is affected by stress hormones
- Bloating and gas — altered motility plus microbiome shifts
- Appetite changes, both suppression and increased emotional eating
- Worsening of existing conditions like IBS, IBD, and GERD under stress
The Microbiome Is Listening
Stress and gut health are linked through the microbiome, where stress reduces beneficial bacteria and increases inflammation.
This is the part that keeps researchers busy. Stress doesn’t just affect how the gut moves — it changes what’s living in it. Studies show that psychological stress reduces microbial diversity, decreases the abundance of Lactobacillus species, and increases gut permeability. And the reverse is also true: gut dysbiosis — an imbalanced microbiome — can independently increase anxiety and mood disturbance through the same gut-brain pathway. It becomes circular. Stress worsens the gut health. The gut worsening feeds back into psychological state.
Managing the Connection
Stress and gut health can be improved through lifestyle changes like healthy eating, proper sleep, and stress management techniques.
You can’t fully separate mental and digestive health — they’re the same system looked at from different angles. Which means treating one without the other misses half the picture. What actually helps:
- Mindfulness and stress reduction practices — with real, measurable effects on gut motility and microbiome composition
- Regular sleep — poor sleep independently disrupts the gut flora and stress hormones
- Dietary support for the microbiome: fermented foods, prebiotic fibers, diverse plant intake
- Exercise — which reduces cortisol and directly improves gut transit
- Cognitive behavioral therapy, particularly for IBS — evidence base is strong here
- Addressing the actual stress sources rather than only managing symptoms
Conclusion
Stress and gut health are inseparable. The gut isn’t just a passive victim of your nervous system — it’s an active participant in how you experience stress and anxiety. If your digestive system has felt off during a rough period of life, that’s not psychosomatic in a dismissive sense. It’s real physiology. And it means healing often needs to happen on both fronts at once.
FAQs
Q1. Can anxiety cause physical stomach pain?
Yes. Visceral hypersensitivity — where the gut becomes more sensitive to normal sensations — is a recognized mechanism. The pain is real, not imagined.
Q2. How quickly can stress affect digestion?
Almost immediately in acute stress. Chronic low-grade stress creates changes over weeks and months, particularly in the microbiome.
Q3. Does meditation actually help with IBS?
There is genuine evidence for mindfulness-based interventions improving IBS symptoms, particularly pain, urgency, and psychological distress.
Q4. Can gut bacteria affect mood?
Yes. The gut-brain axis runs both directions. Specific microbial strains are linked to serotonin production and have been shown to influence anxiety and depression markers.
Q5. Should I see a gastroenterologist or a therapist for stress-related gut problems?
Ideally both. The physical symptoms need evaluation. But treating only the gut without addressing the stress is usually incomplete.







