There’s something about the liver that feels invisible.
You don’t feel it working. You don’t hear it complain. It doesn’t throb dramatically like a headache or tighten like a cramp in your calf. It just… does its job. Quietly. Faithfully. Processing everything you eat, everything you drink, every pill you swallow in a moment of relief.
And yet, when it begins to struggle, the signs are often subtle. A little fatigue. A strange heaviness after meals. Maybe your eyes look slightly yellow in a bathroom mirror at midnight and you tell yourself it’s the lighting.
We are experts at postponing concern.

The topic of liver disease diagnosis doesn’t usually enter conversation until something forces it to. A blood test result. A routine health check-up. An ultrasound report folded in half and opened slowly.
But late at night, when you start thinking about what keeps you alive without applause, the liver feels less like an organ and more like a filter for your entire existence. It carries your excess. Your indulgences. Your habits. Your coping mechanisms.
And when it falters, everything feels slightly off-balance.
This is not a dramatic organ. It doesn’t demand attention. It absorbs damage quietly. That’s part of what makes liver diseases complicated — they can progress without obvious alarms.
Which is why diagnosis matters more than we admit.
What is Liver Diseases & Diagnosis?
Liver diseases are conditions that affect the structure or function of the liver. That sounds textbook. Clean. Contained.
But in reality, liver diseases range widely:
- Fatty liver disease (both alcoholic and non-alcoholic)
- Hepatitis (viral, autoimmune, toxic)
- Cirrhosis
- Liver fibrosis
- Liver cancer
- Genetic metabolic disorders
Each one carries its own story. Its own pace. Its own risks.
The liver itself is a large organ, tucked under the right side of your ribcage. It performs hundreds of functions — detoxification, bile production, protein synthesis, blood clot regulation, nutrient metabolism. It’s less an organ and more a biochemical factory.
Diagnosis, then, is the process of identifying what’s going wrong inside that factory.
Liver disease diagnosis involves piecing together information:
- Blood tests.
- Imaging scans.
- Physical examination.
- Patient history.
- Sometimes, biopsy.
It’s rarely a single dramatic discovery. More often, it’s pattern recognition.
Elevated liver enzymes.
Abnormal bilirubin levels.
Changes seen on ultrasound.
Symptoms that align.
It’s medicine assembling a puzzle.
The tricky part? Many liver diseases are silent in early stages. You can have fatty liver for years without feeling anything specific. You can have mild fibrosis without pain.
By the time symptoms like jaundice, abdominal swelling, or confusion appear, the disease may already be advanced.
That’s the unsettling part.
The liver has remarkable regenerative capacity. It can repair itself. It can regrow. It can compensate. But there is a limit. And diagnosis aims to catch disease before that limit is reached.
liver disease diagnosis through blood tests
- Liver function tests (LFTs)
- ALT (Alanine transaminase)
- AST (Aspartate transaminase)
- Bilirubin levels
- Alkaline phosphatase
- Albumin
- Prothrombin time
Blood tests are often the first whisper of trouble.
You go for a routine check-up. Maybe for something unrelated — fatigue, insurance paperwork, annual health screening. And then the report comes back with slightly elevated ALT or AST.
Mildly raised. Borderline high. Not dramatic.
This is where liver disease diagnosis often begins — in numbers.
ALT and AST are enzymes released into the bloodstream when liver cells are damaged. Elevated levels don’t automatically mean severe disease. They simply mean something is irritating or injuring liver cells.
It could be fatty liver.
It could be medication.
It could be alcohol.
It could be viral hepatitis.
It could be transient.
The nuance matters.
Bilirubin levels tell another story — about bile processing. Albumin and clotting factors reflect the liver’s synthetic function. When these are abnormal, it suggests more advanced dysfunction.
Blood tests don’t give the full picture. They signal direction.
They say: look deeper.
And sometimes that’s enough to change behavior. To reduce alcohol. To modify diet. To investigate further.
Sometimes early intervention begins with one abnormal number.
liver disease diagnosis with imaging
- Ultrasound
- CT scan
- MRI
- FibroScan (transient elastography)
Imaging feels more concrete. More visual.
An ultrasound can detect fatty infiltration. It can show an enlarged liver. It can identify masses, cysts, or irregular texture suggestive of cirrhosis.
CT scans and MRI offer detailed structural information. They reveal lesions. Tumors. Blood flow changes.
FibroScan is more specialized. It measures liver stiffness, which correlates with fibrosis. It’s non-invasive. Quick. Almost anticlimactic for something so informative.
The role of imaging in liver disease diagnosis is to move beyond numbers and into structure.
Because enzymes fluctuate. But scarring leaves evidence.
Fibrosis develops slowly. Scar tissue replaces healthy tissue. And while early fibrosis can be reversible, advanced cirrhosis is not.
Imaging helps stage disease. It helps doctors decide urgency. It clarifies whether lifestyle modification is enough or whether more aggressive treatment is required.
There’s something sobering about seeing an organ’s condition on a screen. It removes ambiguity.
liver disease diagnosis in fatty liver
Fatty liver disease is increasingly common. Sedentary lifestyles. Processed diets. Chronic stress. Excess sugar. Alcohol.
Non-alcoholic fatty liver disease (NAFLD) can exist in people who don’t drink at all.
The challenge in liver disease diagnosis in fatty liver is that it’s often silent.
You might feel tired. Or not.
You might have mild discomfort in the right upper abdomen. Or not.
You might feel completely normal.
Diagnosis often begins with elevated liver enzymes or an incidental finding on ultrasound.

But fatty liver is not always benign. It can progress to non-alcoholic steatohepatitis (NASH), fibrosis, and eventually cirrhosis.
That’s the progression people underestimate.
Early diagnosis matters because fatty liver, especially in early stages, can often be reversed with:
- Weight loss.
- Dietary changes.
- Exercise.
- Reduced alcohol intake.
- Better metabolic control.
The liver can heal — if given the chance.
But without diagnosis, there is no intervention.
liver disease diagnosis in hepatitis
Hepatitis — inflammation of the liver — can be viral, autoimmune, drug-induced, or alcohol-related.
In viral hepatitis (like Hepatitis B or C), diagnosis involves:
- Serological blood tests for viral markers.
- Viral load measurements.
- Liver function tests.
- Imaging if chronic damage is suspected.
The weight of a hepatitis diagnosis feels different. It carries stigma sometimes. Fear. Questions about transmission.
But modern medicine has transformed outcomes. Hepatitis C, once chronic and progressive, is now often curable with antiviral therapy.
The key is identification.
Liver disease diagnosis in hepatitis requires early screening, especially in high-risk individuals. Untreated chronic hepatitis can silently lead to cirrhosis and liver cancer over years.
And again — silence is the theme.
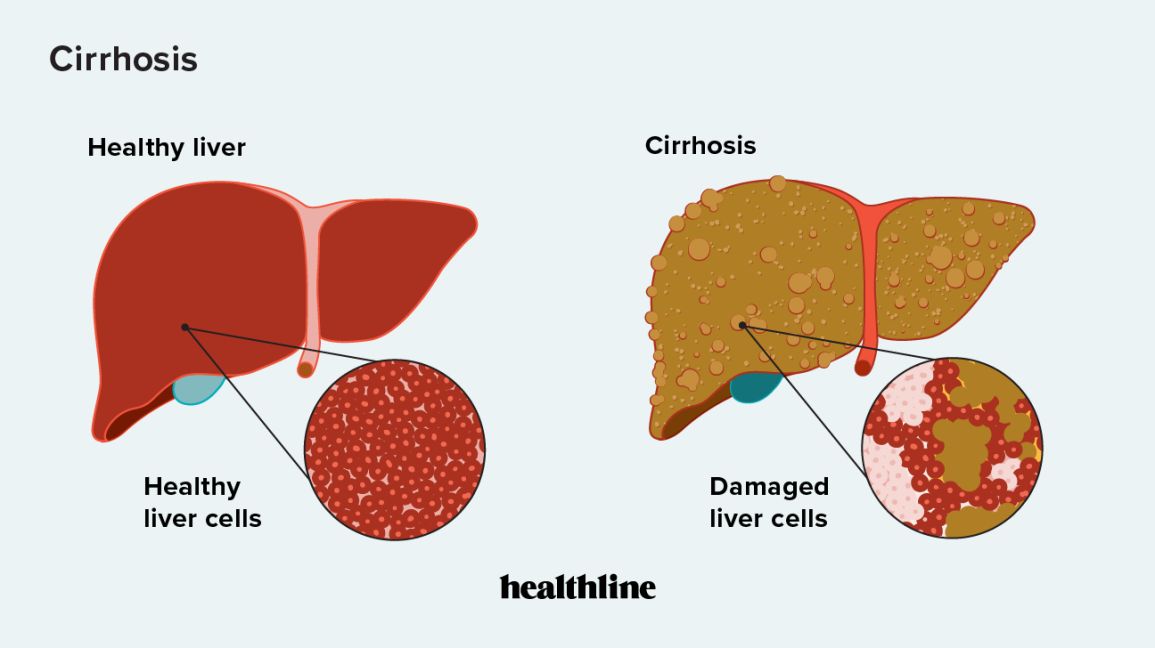
liver disease diagnosis in cirrhosis
Cirrhosis is advanced scarring of the liver.
By the time cirrhosis develops, symptoms may appear:
- Abdominal swelling (ascites)
- Jaundice
- Easy bruising
- Confusion (hepatic encephalopathy)
- Spider-like blood vessels on the skin
But sometimes even cirrhosis is discovered incidentally.
Diagnosis involves blood tests, imaging, and sometimes biopsy. Signs like low platelets, enlarged spleen, and irregular liver contour on ultrasound suggest advanced disease.
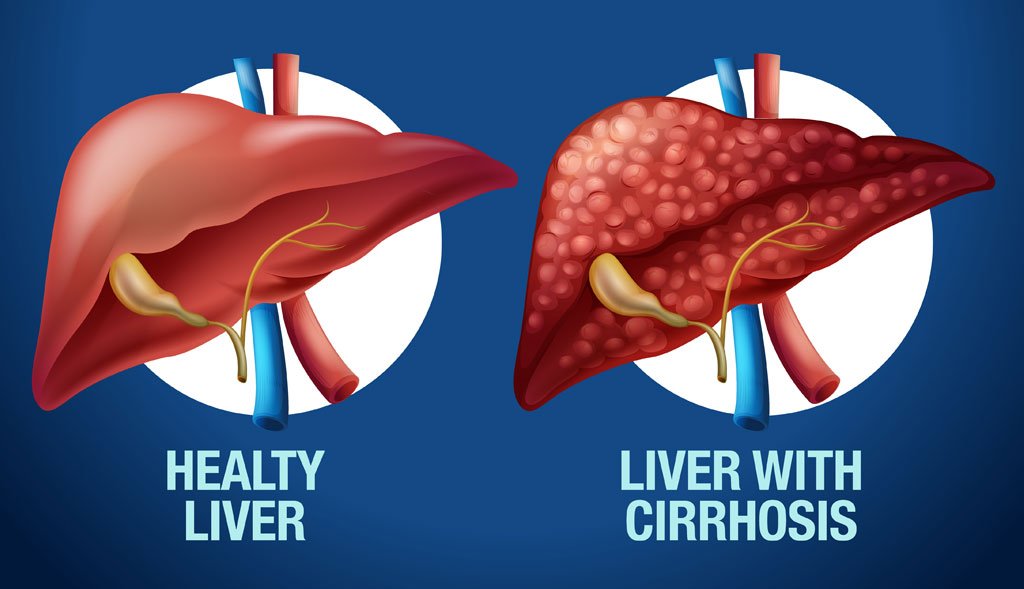
The gravity of liver disease diagnosis in cirrhosis lies in its irreversibility. Early cirrhosis can sometimes stabilize. Advanced cirrhosis may require transplant evaluation.
This is where early detection earlier in the disease spectrum becomes painfully relevant.
Conclusion
The liver is resilient. Remarkably so.
It forgives late nights, dietary excess, stress cycles, occasional indulgences. It regenerates. Repairs. Compensates.
But it is not infinite.
The idea of liver disease diagnosis isn’t about panic. It’s about attention. Awareness. Routine checks that feel boring but are profoundly protective.
Diagnosis is not a verdict. It’s information.
Sometimes it brings relief — normal results.
Sometimes it brings a wake-up call — mild fatty change.
Sometimes it brings urgency.
But it always brings clarity.
And clarity is powerful.
Because once you know, you can act.
FAQs
- What are the early signs of liver disease?
Early stages often have no symptoms. Some people may experience fatigue, mild abdominal discomfort, or unexplained changes in lab results.
- Can liver disease be reversed?
Fatty liver and early fibrosis can often be reversed with lifestyle changes. Advanced cirrhosis is usually not reversible but can sometimes be managed.
- How is liver disease diagnosed?
Through blood tests, imaging (ultrasound, CT, MRI, FibroScan), and sometimes liver biopsy.
- Is liver biopsy always necessary?
No. Many cases can be diagnosed and staged with non-invasive tests. Biopsy is used when diagnosis is uncertain or detailed staging is required.
- How often should I get my liver checked?
If you have risk factors like obesity, diabetes, alcohol use, viral hepatitis, or family history, regular monitoring as advised by your doctor is important. Routine health check-ups often include liver function tests.







