Two Procedures, Two Very Different Parts of You:-
Your doctor says you need a GI procedure. Maybe they said ‘endoscopy.’ Maybe they said ‘colonoscopy.’ Maybe they used both words in the same sentence and then handed you a pamphlet that you haven’t read yet. Either way, you’re now sitting somewhere trying to figure out what the difference between endoscopy and colonoscopy actually is Understanding endoscopy vs colonoscopy helps clarify which part of the digestive system your doctor needs to examine and why the procedure is recommended, and why you need one and not the other, or maybe both, and what any of it involves. Understanding endoscopy vs colonoscopy is important because both procedures examine different parts of the digestive tract and help diagnose different conditions.
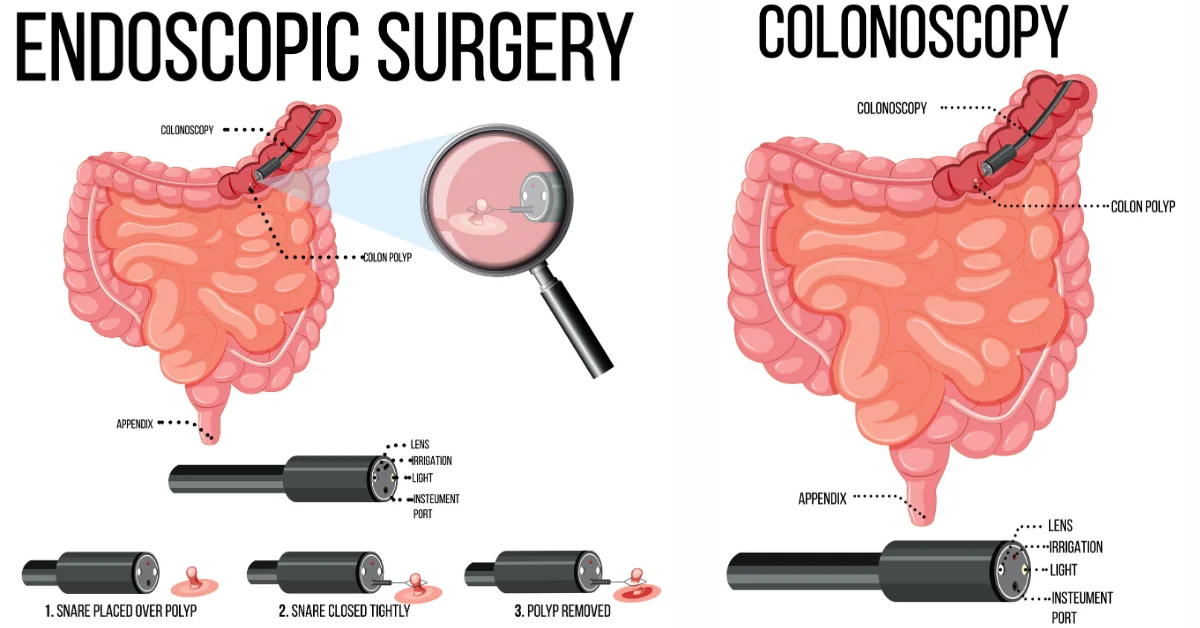
They are not the same thing. They use similar technology — a flexible tube with a camera — but they go in different directions and they’re looking at different parts of the digestive tract for different problems. Understanding which is which isn’t just trivia. It tells you something meaningful about what your doctor is actually worried about.
Endoscopy vs colonoscopy refers to two different medical procedures used to examine the digestive tract. Endoscopy checks the upper digestive system, including the esophagus, stomach, and duodenum, while colonoscopy examines the large intestine and rectum. Both procedures help doctors diagnose digestive disorders, detect bleeding, and identify early signs of gastrointestinal disease.
Endoscopy vs Colonoscopy: What an Endoscopy Examines
When comparing endoscopy vs colonoscopy, the endoscopy focuses on the upper digestive tract including the esophagus, stomach, and duodenum.
An upper GI endoscopy (technically called an esophagogastroduodenoscopy, or EGD — which is why everyone just says endoscopy) examines the upper digestive tract. The scope goes in through the mouth, down the esophagus, into the stomach, and then into the first part of the small intestine called the duodenum.
It’s used to investigate:
- Persistent heartburn or acid reflux that isn’t responding to medication
- Difficulty swallowing (dysphagia)
- Unexplained nausea or vomiting
- Stomach pain, especially upper abdominal pain
- Suspected ulcers — gastric or duodenal
- Bleeding in the upper GI tract
- Screening for Barrett’s esophagus in people with long-term acid reflux
When looking at endoscopy vs colonoscopy, the endoscopy covers the part of the digestive system that processes food first — the path from swallowing to the point where nutrients begin to be absorbed. This is the territory of GERD, ulcers, gastritis, and esophageal conditions.
In some cases, doctors may also recommend additional tests when digestive symptoms are related to liver problems, making early liver disease diagnosis important for proper treatment.
What a Colonoscopy Is — and Why It’s Different
A colonoscopy examines the lower end of the digestive tract — specifically the large intestine (colon) and the rectum. The scope enters through the other end entirely, with the patient lying on their side, and travels backward through the entire length of the colon.
In the discussion of endoscopy vs colonoscopy, colonoscopy specifically examines the large intestine and rectum. In the comparison of endoscopy vs colonoscopy, colonoscopy specifically examines the large intestine and rectum for abnormalities such as polyps or cancer.

It’s looking for:
- Colorectal cancer or precancerous polyps
- Inflammatory bowel disease — Crohn’s disease and ulcerative colitis
- Unexplained lower abdominal pain
- Changes in bowel habits — persistent diarrhea, constipation, or a change in stool caliber
- Blood in the stool or rectal bleeding
- Diverticular disease
The colonoscopy is the gold standard for colon cancer screening and it’s recommended for average-risk adults starting at 45. It’s both diagnostic and therapeutic — polyps can be removed during the procedure itself, in real time, which is part of what makes it uniquely useful.
| Feature | Endoscopy | Colonoscopy |
|---|---|---|
| Examines | Esophagus, stomach, duodenum | Colon and rectum |
| Entry point | Mouth | Rectum |
| Main purpose | Diagnose ulcers, reflux, gastritis | Detect polyps and colon cancer |
| Prep required | Fasting 6–8 hours | Full bowel prep |
| Procedure time | 10–20 minutes | 30–60 minutes |
How the Preparation Differs
Another important difference in endoscopy vs colonoscopy is the preparation required before each procedure. Another important difference between endoscopy vs colonoscopy is the preparation required before the procedure.
This is one of the more practical GI proceduresdistinctions and it matters for anyone planning their schedule.
For an upper endoscopy, prep is relatively simple: nothing to eat or drink for six to eight hours before the procedure. An empty stomach ensures the doctor has a clear view and reduces the risk of aspiration during sedation. That’s mostly it.

For a colonoscopy, the prep is considerably more involved. The colon needs to be completely empty — which means a clear liquid diet the day before and a bowel cleanse using a laxative solution, taken either all the night before or split between the night before and the morning of the procedure. It’s not the most comfortable day. But it’s what makes the colonoscopy accurate. A poorly prepped colon means missed polyps, and missed polyps are the whole problem.
The Procedures Themselves — What Actually
Both are typically done under conscious sedation, sometimes called twilight sedation. You’re not fully under general anesthesia but you’re deeply relaxed and usually have no memory of the procedure. Most people describe waking up and being told it’s already done.
An upper endoscopy takes about 10 to 20 minutes on average. A colonoscopy takes 30 to 60 minutes, longer if polyps are found and removed. Both require someone else to drive you home because of the sedation.
Recovery from both is generally quick. With an endoscopy you might have a mild sore throat for a day. With a colonoscopy you’ll likely experience some bloating and gas as the air used to inflate the colon works its way out — completely normal, resolves within a few hours.
Can You Need Both at the Same Time
Yes. In fact, having both procedures done on the same day under the same sedation is not uncommon. If a patient has symptoms suggesting both upper and lower GI issues — say, chronic heartburn alongside rectal bleeding — a gastroenterologist may recommend doing both in a single session. This is called a bidirectional endoscopy, and it reduces the number of times you have to deal with sedation and recovery.
The prep is still the colonoscopy prep in that case, since both require an empty GI tract. In some situations, doctors may recommend both procedures together when symptoms suggest issues in both areas, making the endoscopy vs colonoscopy comparison relevant for diagnosis.
Which One Do You Actually Need
Deciding between endoscopy vs colonoscopy depends on the symptoms and the part of the digestive system that needs evaluation.
This isn’t really a self-determination question. Your symptoms and your doctor’s clinical judgment guide the decision. But as a general orientation:
- Upper abdominal symptoms — heartburn, reflux, nausea, swallowing difficulty, ulcer pain — point toward endoscopy
- Lower abdominal symptoms — bowel habit changes, lower abdominal pain, rectal bleeding — point toward colonoscopy
- Routine cancer screening at age 45 (or earlier with family history) means colonoscopy
- Blood in vomit or black tarry stools — upper GI bleed — means urgent endoscopy
- Bright red rectal bleeding — lower GI issue — warrants colonoscopy
When the symptoms are ambiguous or systemic — unexplained weight loss, severe fatigue, anemia — the gastroenterologist may want to look at both ends.
Persistent digestive symptoms such as abdominal discomfort, changes in bowel habits, or chronic bloating after meals may require medical evaluation through procedures like endoscopy or colonoscopy.
Risks and What to Reasonably Expect
Both procedures carry low but real risks. For endoscopy: perforation of the esophagus or stomach (rare, approximately 1 in 2500), bleeding if a biopsy or therapeutic intervention is performed, reactions to sedation. For colonoscopy: perforation (approximately 1 in 1000), post-polypectomy bleeding (1 in 200 to 500), sedation-related effects. Some digestive symptoms investigated through endoscopy may also be linked to liver conditions, including the early signs of fatty liver disease.
These numbers are small. The risk of not investigating persistent GI symptoms — or skipping routine colon cancer screening — is meaningfully larger for most people. That’s the clinical calculation your doctor is making.
Maintaining digestive health through proper nutrition is also important for preventing gastrointestinal disorders. Following the right diet tips for gut health can support better digestion and overall gut function.
About Dr. Vibhor Pareek – A Specialist in Gastroenterology
The Advanced Gastro Care Clinic is run by Dr. Vibhor Pareek, a specialist in gastroenterology who is committed to offering quality health care to patients dealing with stomach problems and liver ailments. At this clinic, patients can expect accurate diagnoses, ethical medical practices, and a comfortable experience throughout their treatment.
Dr. Pareek offers treatment for a variety of stomach problems, including those affecting the liver, as well as endoscopic procedures. By employing modern technology in medicine, this clinic ensures that patients are given proper guidance and treatment.
With a strong foundation in trust, transparency, and stomach health, the Advanced Gastro Care Clinic is committed to helping patients overcome stomach problems, including liver ailments, with confidence and guidance.
Conclusion
The endoscopy vs colonoscopy question comes down to location. Upper tract symptoms, upper GI problems — endoscopy. Lower tract symptoms, colon health, cancer screening — colonoscopy. Both are outpatient procedures, both involve sedation, both are brief and generally well-tolerated. The difference between them isn’t scary, it’s just anatomical. Knowing which one you’re having, and why, makes the whole process feel a lot less like something happening to you and more like something being done for you. The difference between endoscopy vs colonoscopy mainly comes down to which part of the digestive system needs examination.
Frequently Asked Questions
- Is an endoscopy more painful than a colonoscopy?
Neither is typically painful because both are done under conscious sedation. You may have a mild sore throat after an endoscopy and some bloating after a colonoscopy, but significant pain during either procedure is not a normal experience.
- What is the main difference between endoscopy and colonoscopy?
An endoscopy examines the upper digestive tract — esophagus, stomach, and upper small intestine — via the mouth. A colonoscopy examines the large intestine via the rectum. They investigate different parts of the GI system for different conditions.
- Do I need to fast before both procedures?
For an endoscopy, fasting for six to eight hours is typically sufficient. For a colonoscopy, a more extensive bowel prep the day before is required, including a clear liquid diet and laxative solution.
- How long does each procedure take?
An upper endoscopy typically takes 10 to 20 minutes. A colonoscopy takes 30 to 60 minutes, potentially longer if polyps are removed. Both require additional time for check-in, prep, and post-procedure recovery before discharge.
- Can both procedures be done on the same day?
Yes. Bidirectional endoscopy — performing both an upper endoscopy and a colonoscopy in the same session under the same sedation — is a common practice when symptoms suggest issues in both the upper and lower GI tract.







