The Organ You Never Think About Until It’s Too Late
The liver is a quiet organ. It doesn’t send you pain signals early. It doesn’t protest loudly when things start going wrong. It just keeps working, compensating, doing its job in near silence — until the point where it can’t anymore. The early signs of fatty liver disease often develop silently, which is why many people don’t realize they have it until the condition progresses.
The thing that’s alarming about this — if you want to call it alarming, and honestly you probably should — is how common it’s become. Non-alcoholic fatty liver disease (NAFLD) now affects roughly a quarter of the global population. A quarter. It’s not a rare condition. It’s happening in people who eat reasonably, who don’t drink excessively, who don’t think of themselves as someone with a liver problem.
Early signs of fatty liver disease include fatigue, discomfort in the upper right abdomen, brain fog, and elevated liver enzymes. These symptoms often appear slowly and may go unnoticed for years.
What Happens to the Liver in the Early Signs of Fatty Liver Disease
Understanding the early signs of fatty liver disease starts with knowing how fat builds up in the liver. During the early signs of fatty liver disease, fat begins to accumulate inside liver cells. While a small amount of fat in the liver is normal, excessive fat buildup can gradually affect how the liver functions. Following the right diet tips for gut health can also support liver function and reduce fat buildup in the liver.

. Everyone has a little fat in their liver — that’s normal. The problem starts when fat comprises more than five to ten percent of the liver’s weight. At that point, the organ starts to function differently.
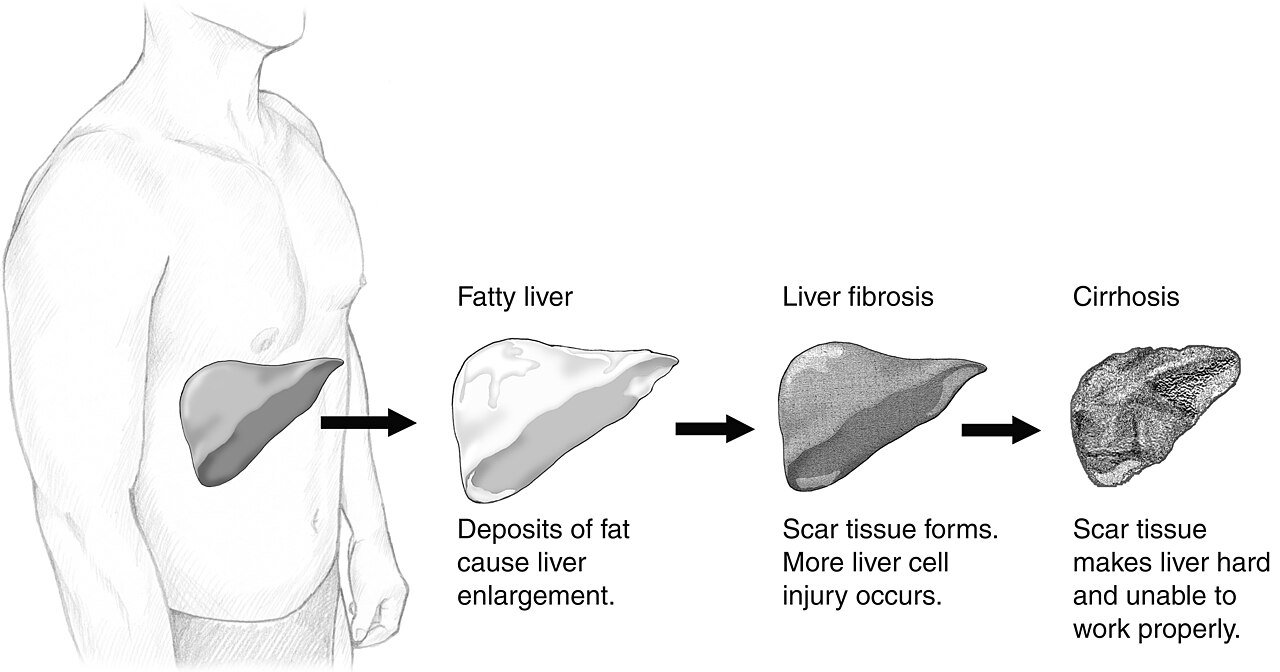
Left alone, fatty liver symptoms can progress. The stages go: simple fatty liver (steatosis) → non-alcoholic steatohepatitis (NASH, which means the fat is causing inflammation) → fibrosis (scarring) → cirrhosis (extensive, irreversible scarring) → liver failure or liver cancer. This progression doesn’t happen overnight. It can take decades. But it also doesn’t always announce itself along the way.
Early Signs of Fatty Liver Disease — What to Watch For
Here’s the frustrating part. Early signs of fatty liver disease are often vague. Generic. Easy to attribute to other things — stress, poor sleep, age, a bad week. The early signs of fatty liver disease are often subtle and easy to ignore.
Still, they’re worth knowing:
- Fatigue — not just tiredness, but a heaviness that doesn’t improve with sleep. The liver is involved in energy metabolism, and when it’s compromised, you feel it
- Discomfort in the upper right abdomen — a dull ache or feeling of fullness in the area just below the ribs on the right side, where the liver sits
- Unexplained weight gain, particularly around the abdomen, often alongside insulin resistance
- Brain fog — difficulty concentrating, mental sluggishness. The liver processes toxins; when that slows, cognitive effects can appear
- Elevated liver enzymes on a blood test — often the first actual medical signal, and one that still gets dismissed as ‘mildly elevated, let’s watch it’
- Nausea, especially after fatty meals
Many of these symptoms may appear mild, but they can still indicate the early signs of fatty liver disease developing silently.
Many people have no symptoms at all until the disease has progressed. That’s not a comforting fact. It’s a reason to be more proactive about liver health tips and routine screening, especially if risk factors are present.
Because early symptoms are often mild, proper liver disease diagnosis through blood tests and imaging becomes essential for identifying liver problems at an early stage.
Who Is Actually at Risk
People with metabolic risk factors are more likely to experience the early signs of fatty liver disease.
Risk factors for fatty liver symptoms include:
- Obesity, especially central obesity (fat concentrated around the midsection)
- Type 2 diabetes or insulin resistance
- High triglycerides or low HDL cholesterol
- Metabolic syndrome
- Hypothyroidism
- Polycystic ovarian syndrome (PCOS)
- A sedentary lifestyle
- Rapid weight loss (counterintuitive, but crash dieting can worsen fatty liver)
- Certain medications — corticosteroids, amiodarone, tamoxifen
You don’t have to check every box. One or two of these, alongside the vague symptoms above, is enough to warrant a conversation with your doctor.

Why Fatty Liver Gets Missed for So Long
Part of it is that there are no early, loud symptoms. Part of it is that liver enzyme tests — AST, ALT — are often run as part of routine bloodwork, but mildly elevated results get noted and then not followed up on seriously. And part of it is that people don’t know their liver is even something to monitor unless they drink heavily or have hepatitis.
The cultural script around liver disease is alcohol. If you don’t drink much, the idea that your liver could be accumulating fat from diet, metabolic dysfunction, insulin resistance — it just doesn’t cross most people’s minds. And it doesn’t cross a lot of doctors’ minds to flag it proactively either.
An ultrasound of the abdomen can show fatty liver quite clearly. It’s a standard diagnostic tool, not invasive, not expensive. But it requires someone to order it. And that requires someone to look at the full picture — the weight, the waist circumference, the blood sugar, the triglycerides — and connect the dots.
Fatty Liver Prevention — What Actually Moves the Needle
If detected early, the early signs of fatty liver disease can often be reversed with lifestyle changes. The good news, and it is genuinely good news, is that fatty liver prevention is very much possible. And in the early stages, the condition is reversible. The liver has remarkable regenerative capacity. Intervene early enough and the fat comes down, the enzymes normalize, the risk of progression drops significantly.
What works:
- Weight loss of 5-10% — this alone can significantly reduce liver fat content. The relationship is that direct
- Dietary changes — reducing refined carbohydrates (especially fructose and sugar-sweetened beverages), processed foods, and saturated fats. The Mediterranean diet consistently comes out ahead in the research
- Regular aerobic exercise — even without weight loss, exercise reduces liver fat. Both aerobic and resistance training help, but aerobic exercise shows more direct impact on liver fat specifically
- Controlling blood sugar — if insulin resistance or type 2 diabetes is present, managing it aggressively matters enormously for liver health
- Limiting alcohol — even in non-alcoholic fatty liver disease, alcohol accelerates progression. This one requires honesty about how much is actually being consumed
- Coffee — genuinely one of the most consistent findings in liver research. Regular coffee consumption (even just two cups daily) is associated with reduced risk of liver fibrosis and lower liver enzyme levels. Mechanism is still being studied but the signal is strong
There’s no approved medication specifically for NAFLD yet, though several are in late-stage trials. What exists are treatments for the associated conditions — diabetes management, lipid-lowering drugs, weight management support. The primary liver health tips remain lifestyle-based.
The Progression You’re Trying to Avoid
NASH is the inflamed version of fatty liver. Once inflammation enters the picture, damage accelerates. Fibrosis — scar tissue — starts to form. The liver becomes stiffer, less functional. This is the stage where things can become genuinely serious, and where reversal becomes harder rather than straightforward.
Cirrhosis is the endpoint nobody wants. At that stage, the damage is structural. The liver can still function to a degree but it’s compromised significantly and the risk of liver cancer (hepatocellular carcinoma) rises substantially. The goal of all the early intervention — the diet changes, the exercise, the blood sugar control — is specifically to prevent reaching this point.
Conclusion
Recognizing the early signs of fatty liver disease early can make a major difference in preventing long-term liver damage, but it doesn’t stay open forever. The early signs of fatty liver disease are quiet and easy to miss, which makes proactive awareness more important than reactive response. If you have metabolic risk factors — if you carry weight around your midsection, if your blood sugar trends high, if your triglycerides are elevated — take your liver seriously before it has reason to complain.
Routine blood tests. An ultrasound if your doctor thinks it’s warranted. And the unglamorous but genuinely effective interventions: real food, less sugar, consistent movement. It’s not complicated. It’s just consistent.
Frequently Asked Questions
-
Can fatty liver disease be reversed?
Yes, in the early stages (simple steatosis and even early NASH), fatty liver is reversible through dietary changes, weight loss, exercise, and metabolic management. The liver has strong regenerative capacity. Later-stage fibrosis and cirrhosis cannot be fully reversed.
-
What are the early signs of fatty liver disease to look out for?
Most people have no symptoms early on. When symptoms do appear they often include fatigue, discomfort in the upper right abdomen, and brain fog. The most common early finding is mildly elevated liver enzymes on a blood test.
-
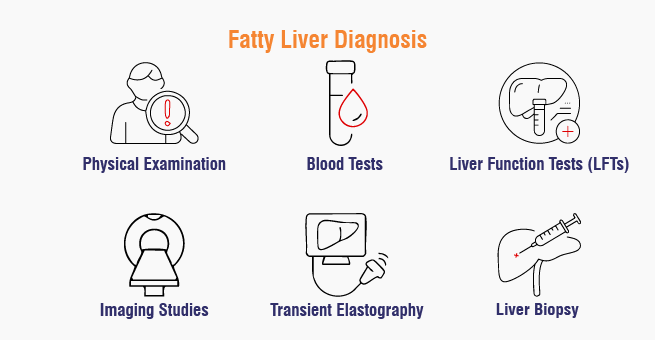
How is fatty liver diagnosed?
The most common methods are blood tests (liver enzymes ALT and AST), ultrasound imaging, and increasingly, non-invasive tests like FibroScan (transient elastography) that measure liver stiffness. A biopsy is the gold standard but is usually reserved for cases where NASH or advanced fibrosis needs to be confirmed.
-
Does alcohol cause non-alcoholic fatty liver disease?
No — NAFLD by definition occurs in people who drink little to no alcohol. However, alcohol does worsen any existing fatty liver condition and accelerates progression. People diagnosed with NAFLD are generally advised to minimize or eliminate alcohol.
-
Is fatty liver disease hereditary?
There is a genetic component — certain gene variants (like PNPLA3) increase susceptibility. But lifestyle and metabolic factors are the dominant drivers. A family history raises risk but lifestyle modification still makes a substantial difference.







