A little discomfort. A little fatigue. A subtle change in routine that you dismiss because you’re busy, because work is waiting, because life doesn’t pause for digestive irregularities. We are brilliant at ignoring signals. Especially when those signals come from somewhere we don’t like to talk about.
The colon.
Even the word feels clinical. Quiet. Slightly uncomfortable.
But tonight, when everything is still and the distractions thin out, it becomes easier to sit with it. To admit that health isn’t just about the visible parts. It’s about the hidden tunnels too. The winding, patient passageways inside you that have been working nonstop since you were born.
And somewhere in that quiet reflection, the phrase colonoscopy importance starts to make sense in a different way. Not as a medical slogan. Not as a hospital pamphlet. But as a checkpoint. A pause. A flashlight inside a dark corridor.
Because sometimes what we don’t see is exactly what we need to look at.
What is Colonoscopy?
A colonoscopy is a medical procedure. Yes. Technically speaking.
But in a more human way, it is a visual conversation with your large intestine.
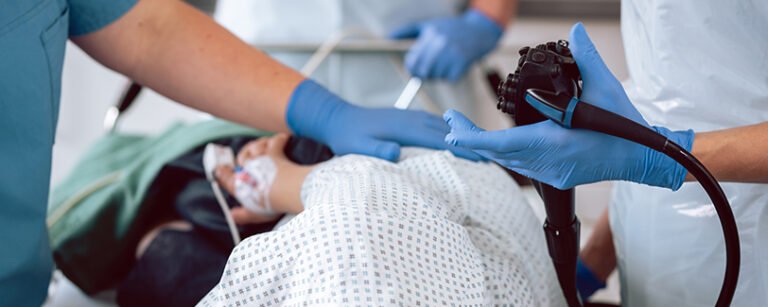
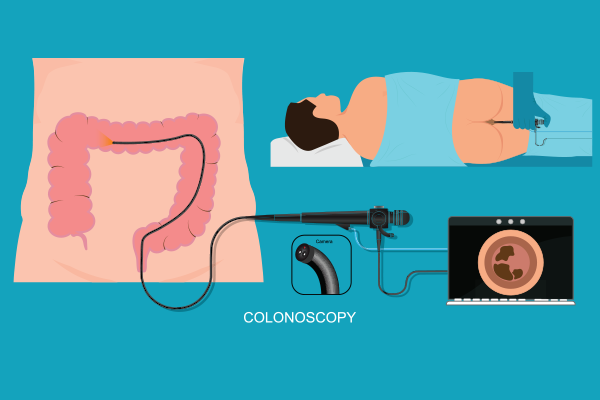
A thin, flexible tube with a camera — called a colonoscope — is gently inserted through the rectum and advanced through the colon. The camera projects images onto a screen. Your doctor watches. Observes. Studies.
It sounds invasive when described plainly. And it is, in a physical sense. But it is also precise. Controlled. Intentional.
During a colonoscopy:
- The entire colon is examined.
- Polyps (small growths) can be detected.
- Suspicious tissue can be biopsied.
- Polyps can often be removed immediately.
- Early signs of cancer can be caught before symptoms appear.
That’s the part that matters.
Before symptoms appear.
Because colorectal cancer often grows quietly. Slowly. Without announcing itself. No dramatic entrance. No immediate pain. Just silent progression.
And a colonoscopy interrupts that silence.
Preparation involves cleaning out the colon — a process that people often dread more than the procedure itself. There’s a liquid diet. A bowel prep solution. Frequent bathroom visits. It’s inconvenient. It’s uncomfortable. It’s temporary.
The procedure itself? Usually done under sedation. You’re relaxed. Sometimes barely aware. It typically lasts 20 to 45 minutes.
And then you wake up. Slight bloating. A little groggy. But done.
It feels almost anticlimactic considering what it can prevent.
Colonoscopy importance
The phrase sounds formal. Clinical. Almost like a textbook heading.
But the colonoscopy importance isn’t academic. It’s personal.
It matters because colorectal cancer is one of the most common cancers worldwide. It matters because early-stage colorectal cancer often has no symptoms. It matters because when detected early, it is highly treatable. When detected late, the story changes.
The importance lies in timing.
A colonoscopy doesn’t just detect cancer. It prevents it.
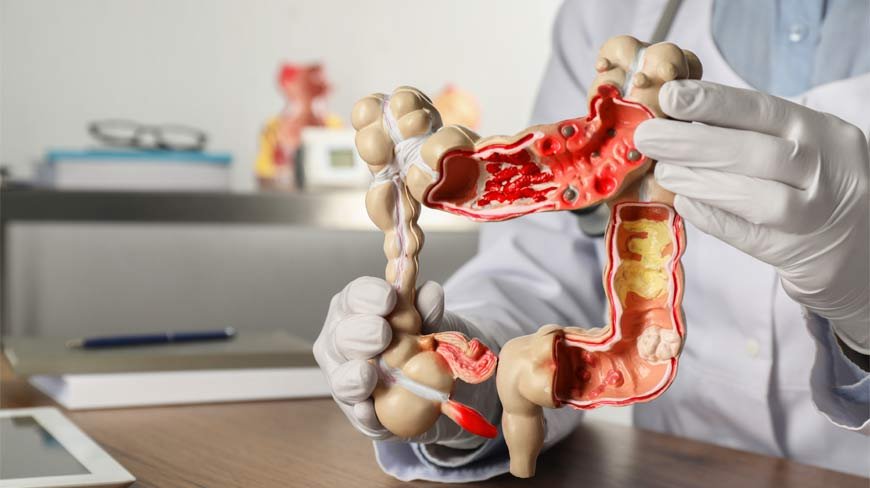
Most colorectal cancers begin as polyps. Not all polyps are dangerous. Some are harmless. But some evolve. Over years. Quietly. Gradually.
And during a colonoscopy, those polyps can be removed.
That’s the quiet miracle.
It’s not just about finding disease. It’s about stopping it before it becomes something heavier.
There’s something powerful about prevention. About stepping ahead of something rather than reacting to it. About choosing discomfort now to avoid devastation later.
And yet… many people postpone it.
Out of embarrassment.
Out of fear.
Out of “I feel fine.”
But feeling fine isn’t always evidence of being fine.
That’s part of the colonoscopy importance we don’t talk about enough — the humility it requires. The willingness to look where we’d rather not. The decision to prioritize long-term health over short-term comfort.
Colonoscopy importance for early detection
If there’s one phrase that keeps echoing in every medical guideline, it’s early detection.
And not in a dramatic way. In a practical one.
- Early-stage colorectal cancer often has no noticeable symptoms.
- Survival rates are significantly higher when cancer is caught early.
- Screening can detect precancerous growths before they become malignant.
That last point matters.
Because this isn’t just a diagnostic tool. It’s preventive medicine in motion.
The colonoscopy importance for early detection becomes clearer when you look at statistics. Five-year survival rates for localized colorectal cancer are high. Once it spreads? They drop.
It’s not about fear-mongering. It’s about perspective.
A colonoscopy sees what you can’t feel. It identifies what blood tests may not reveal. It visually confirms the health of your colon in real time.
There’s something oddly reassuring about that. About seeing proof instead of guessing.
Especially in a world where we Google symptoms at midnight and spiral.
This is different. This is evidence-based reassurance.
Colonoscopy importance after 50
For decades, 50 was the magic number.
Doctors recommended starting routine colonoscopies at age 50 for average-risk individuals. Recently, many guidelines have lowered that age to 45. But the phrase colonoscopy importance after 50 still carries weight because risk increases with age.
As we age:
- Cellular mutations accumulate.
- The likelihood of polyp formation rises.
- The body’s repair mechanisms aren’t as efficient as they once were.
After 50, the statistical curve shifts. The probability of colorectal cancer increases. It doesn’t guarantee anything. It just increases likelihood.
And screening becomes less optional and more essential.
There’s a strange emotional layer to turning 50. It’s a milestone. A midpoint. A reminder that the body has been working hard for decades.
A colonoscopy at this stage feels less like a medical test and more like maintenance. Like checking the foundation of a house that has stood strong for years.
Quiet care. Responsible attention.
Not dramatic. Just wise.
Colonoscopy importance with family history
Family history changes everything.
If a parent, sibling, or close relative has had colorectal cancer or advanced polyps, your risk is higher. Not dramatically guaranteed. But elevated.
And the colonoscopy importance with family history becomes urgent rather than optional.
Genetics carry patterns. Tendencies. Sometimes mutations that quietly pass through generations.
In these cases:
- Screening may begin earlier than 45 or 50.
- Colonoscopies may be recommended more frequently.
- Vigilance becomes part of routine health planning.
It’s not about inheriting fate. It’s about inheriting awareness.
There’s something empowering about knowing your risk profile. About acting on information rather than fearing it.
When there’s family history, a colonoscopy becomes less of a general recommendation and more of a protective boundary.
A line drawn in advance.
Colonoscopy importance in digestive symptoms
Now this part feels more immediate.
Because sometimes the body doesn’t whisper. It nudges. Repeats. Persists.
Symptoms like:
- Rectal bleeding.
- Persistent abdominal pain.
- Unexplained weight loss.
- Changes in bowel habits.
- Iron-deficiency anemia without clear cause.
These are not things to ignore.
The colonoscopy importance in digestive symptoms is about investigation. Clarity. Not jumping to worst-case scenarios — but not dismissing patterns either.
A colonoscopy can diagnose:
- Inflammatory bowel disease.
- Ulcerative colitis.
- Crohn’s disease.
- Polyps.
- Tumors.
- Sources of bleeding.
It’s not always cancer. Often it isn’t. But the procedure answers questions that speculation cannot.
And sometimes relief comes not from good news — but from certainty.
From knowing.
Colonoscopy importance in preventing colorectal cancer
This might be the most powerful aspect.
Prevention.
The colonoscopy importance in preventing colorectal cancer lies in the removal of precancerous polyps during the procedure itself.
It’s almost poetic, in a clinical way.
You go in to look.
You find something small.
You remove it.
And you potentially prevent years of disease.
That’s not dramatic exaggeration. That’s biology.
Most colorectal cancers develop from adenomatous polyps over 10 to 15 years. That’s a long window. A generous warning period. A stretch of time where intervention is possible.
A colonoscopy uses that window.
There’s something deeply reassuring about that timeline. About knowing the body gives clues — and medicine has tools to respond.
Prevention feels less flashy than treatment. It doesn’t get the same emotional storytelling. But it’s quieter. Stronger.
A decision made in advance.
Conclusion
Maybe the reason colonoscopy conversations feel uncomfortable is because they force us to confront vulnerability.
To admit that we are not invincible.
That health requires maintenance.
That ignoring something doesn’t make it disappear.
But if you sit with it — really sit with it — the colonoscopy importance isn’t about fear. It’s about agency.
It’s about choosing knowledge over uncertainty.
Prevention over reaction.
Responsibility over avoidance.
A colonoscopy is not dramatic. It’s not glamorous. It’s not something you post about.
It’s quiet. Private. Practical.
And sometimes that’s exactly what long-term health looks like.
Not loud heroics.
Just steady decisions.
FAQs
- At what age should I get my first colonoscopy?
For average-risk individuals, screening is generally recommended starting at age 45. If there is family history or other risk factors, your doctor may suggest starting earlier.
- How often do I need a colonoscopy?
If results are normal and you are at average risk, it’s usually every 10 years. If polyps are found or risk is higher, the interval may be shorter.
- Is a colonoscopy painful?
Most people are sedated during the procedure and do not feel pain. Mild bloating or cramping afterward is possible but temporary.
- What are the risks of a colonoscopy?
Complications are rare but can include bleeding, perforation, or reactions to sedation. For most people, the benefits outweigh the risks.
- Can lifestyle changes replace the need for a colonoscopy?
Healthy diet, exercise, and avoiding smoking reduce risk — but they do not replace screening. A colonoscopy directly examines and removes precancerous growths, which lifestyle alone cannot do.







