When It Stops Being Occasional and Starts Being Your Life:-
This article explains persistent heartburn causes and what they mean for your health. Most people have had heartburn. That burning in the chest after a big meal, the acidic taste creeping up the throat at two in the morning, the discomfort that follows a glass of wine or a plate of something too rich or too spicy. That kind of heartburn — isolated, situational — is unpleasant but unremarkable. Your body processed something badly and is making its protest known. It passes.

Persistent heartburn is different. It’s not the occasional incident. It’s showing up multiple times a week, sometimes daily, sometimes regardless of what you ate or didn’t eat. It affects sleep. It affects your relationship with food. And it tends to be quietly endured for a very long time before people seek help, often because heartburn feels like a minor complaint even when it’s stopped being minor at all. Many people ignore persistent heartburn causes until symptoms start affecting sleep and daily comfort.
Persistent heartburn is usually caused by GERD, where stomach acid flows back into the esophagus. Common causes include obesity, hiatal hernia, late-night eating, and smoking. Treatment includes lifestyle changes, medications like PPIs, and in severe cases, surgery.
What Is Actually Happening in Your Body
At the lower end of the esophagus there’s a ring of muscle called the lower esophageal sphincter. Its job is to open to let food pass into the stomach and then close tightly so stomach acid stays where it belongs. When this muscle is weakened or relaxed at the wrong time, stomach acid flows back up into the esophagus — a process called acid reflux. The esophagus has no protective lining against acid the way the stomach does. So it burns. Understanding persistent heartburn causes helps explain why acid reflux happens so frequently in some people.
When this reflux happens frequently — more than twice a week, persistently — it crosses the threshold into what’s clinically called GERD: gastroesophageal reflux disease. GERD symptoms and persistent heartburn causesare intertwined but not identical. GERD is the underlying condition. Persistent heartburn is its most recognizable symptom.
The Causes — More Than Just Spicy Food
Understanding persistent heartburn causes means looking beyond just diet. Yes, certain foods relax the lower esophageal sphincter or increase acid production. Looking deeper into persistent heartburn causes reveals that lifestyle and structural issues play a major role. But the causes of persistent, chronic heartburn are often structural, habitual, and sometimes metabolic.
The most common persistent heartburn causes include:

- Hiatal hernia — when part of the stomach pushes up through the diaphragm into the chest cavity, it compromises the sphincter’s ability to keep acid down. Very common in people over 50 and often goes undiagnosed for years
- Obesity — increased abdominal pressure pushes stomach contents upward. The correlation between excess weight and GERD is direct and well-documented
- Pregnancy — the growing uterus creates upward pressure on the stomach; hormonal changes also relax the lower esophageal sphincter
- Delayed gastric emptying — when the stomach empties too slowly (gastroparesis), food and acid stay there longer and the likelihood of reflux increases
- Certain medications — calcium channel blockers, nitrates, some asthma medications, NSAIDs, and bisphosphonates can worsen or trigger reflux
- Smoking — weakens the lower esophageal sphincter, increases acid production, and impairs the natural protective mechanisms of the esophagus
- Eating habits — eating large volumes at once, eating within two to three hours of lying down, eating quickly
- The most common persistent heartburn causes include.
The Symptoms That Go Beyond the Obvious Burn
The chest burn is the one everyone knows. But GERD symptoms can present in ways that seem unrelated to digestion. This is one reason it gets misdiagnosed or missed entirely for years. These symptoms are often linked to underlying persistent heartburn causes that go unnoticed for years.
The wider symptom picture includes:
- Regurgitation — acid or partially digested food coming back into the mouth
- Chronic cough — particularly at night or after meals, sometimes misdiagnosed as asthma or a post-nasal drip problem
- Laryngitis or hoarseness — acid reaching the vocal cords causes irritation
- A persistent sensation of something stuck in the throat (globus sensation)
- Dental erosion — stomach acid repeatedly reaching the mouth erodes enamel over time
- Sleep disruption — lying flat makes reflux more likely; many GERD sufferers wake repeatedly at night
- Chest pain that mimics cardiac pain — this one warrants investigation to rule out heart issues before attributing it to reflux
The constellation of symptoms matters. Someone with chronic cough, mild hoarseness, and disrupted sleep might have ‘silent reflux’ (laryngopharyngeal reflux) without the classic chest burn at all.
When Persistent Heartburn Becomes Something More Serious
Most people with GERD manage it long-term without developing complications. But untreated, persistent acid exposure to the esophagus can lead to real problems. Barrett’s esophagus — a change in the cells lining the lower esophagus in response to chronic acid damage — affects roughly 10 to 15 percent of people with long-term GERD and carries a small but meaningful increased risk of esophageal adenocarcinoma. Untreated persistent heartburn causes can lead to complications like Barrett’s esophagus
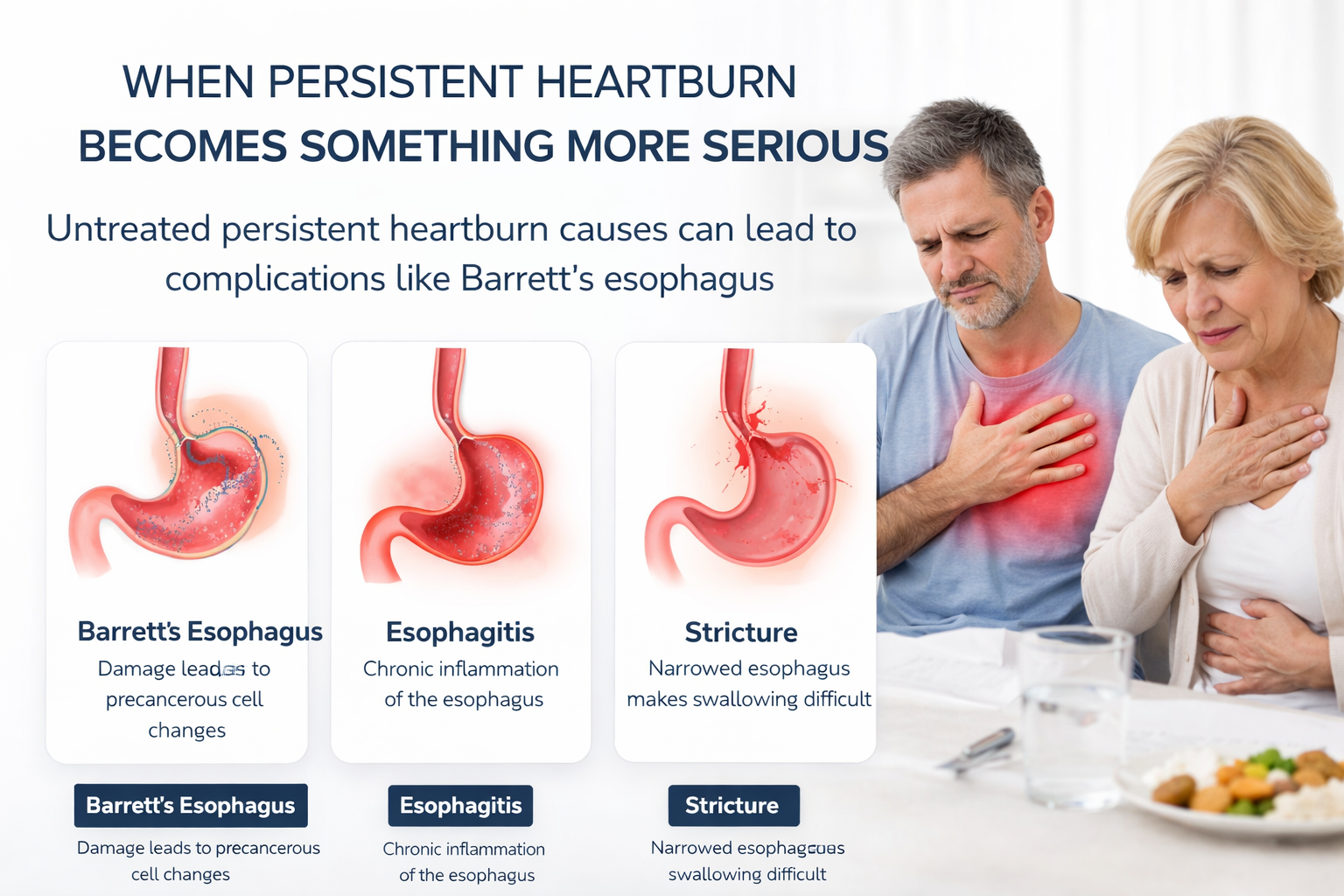
Esophagitis (inflammation), strictures (narrowing that causes progressive swallowing difficulty), and erosions are other complications of chronic, untreated reflux.
This is why ‘just take an antacid and live with it’ is not a good long-term strategy when heartburn is happening multiple times a week.
Treatment Options That Actually Work
Heartburn treatment is layered. It starts with lifestyle and, depending on severity, involves medication. In some cases, procedures or surgery are appropriate. Effective treatment depends on identifying the root persistent heartburn causes rather than just managing symptoms.
Lifestyle interventions that have real evidence behind them:
- Elevating the head of the bed by six to eight inches — not adding pillows (that flexes the body and can worsen reflux), but raising the actual head of the mattress
- Not eating within two to three hours of lying down — gives the stomach time to empty before the prone position makes reflux easier
- Weight loss — even a modest reduction in weight significantly reduces GERD symptoms in overweight individuals
- Avoiding specific triggers — alcohol, caffeine, chocolate, fatty foods, citrus, tomatoes, peppermint. The trigger list varies between people but identifying yours and genuinely reducing exposure matters
- Eating smaller, more frequent meals rather than large ones
- Quitting smoking — this one improves esophageal sphincter function and reduces acid production simultaneously
Improving gut health can also reduce symptoms — explore the best diet for IBS and foods to avoid for better digestion.
Medications:
- Antacids — neutralize acid quickly but briefly; for situational use, not chronic management
- H2 blockers (famotidine, cimetidine) — reduce acid production; work over hours; good for moderate symptoms
- Proton pump inhibitors (PPIs) (omeprazole, pantoprazole, esomeprazole) — the most effective medical treatment for GERD; reduce acid production significantly; taken daily, usually before the first meal
PPIs are effective but not meant to be taken indefinitely without reassessment. Long-term use has associated risks (magnesium deficiency, bone density effects, potential kidney effects) that should be weighed with your doctor.
For patients with confirmed hiatal hernia or severe GERD not responding to medication, surgical options like laparoscopic Nissen fundoplication — where the top of the stomach is wrapped around the esophageal sphincter — can provide long-term resolution.
Diagnosis — What Your Doctor Is Looking For
Persistent heartburn is often diagnosed clinically — meaning based on your symptom history alone. But if symptoms are severe, atypical, or haven’t responded to treatment, further investigation is warranted. If symptoms are complex or persistent, understanding advanced diagnostic methods is important — you can read more about liver disease diagnosis and early detection tests.

An upper endoscopy allows direct visualization of esophageal damage, inflammation, or Barrett’s changes. Ambulatory pH monitoring — where a probe or capsule measures acid exposure in the esophagus over 24 to 48 hours — is the most accurate diagnostic tool for quantifying reflux. Esophageal manometry tests the pressure and function of the esophagus itself.
These are not tests everyone needs. But for complex cases, atypical presentations, or pre-surgical evaluation, they provide information that a symptom history alone cannot.
Conclusion
Understanding persistent heartburn causes is the first step toward long-term relief — hiatal hernia, obesity, diet, smoking, delayed gastric emptying — are things that can be addressed. Heartburn treatment works, but it requires more than just managing symptoms as they arise. Understanding what’s driving the reflux, making the lifestyle changes that actually move the needle, and using medication appropriately (not just indefinitely) — that’s the actual path through this.
The esophagus is not built to handle acid repeatedly over years. Taking persistent reflux seriously isn’t being anxious about a minor problem. It’s protecting a part of your body that doesn’t have a way to protect itself. Addressing persistent heartburn causes early can prevent long-term complications and improve quality of life.
Frequently Asked Questions
- How do I know if my heartburn is GERD?
If heartburn is happening two or more times a week on a regular basis, affects your sleep or daily activities, or isn’t adequately controlled by over-the-counter antacids, it likely meets the threshold for GERD. A doctor can confirm this through your symptom history and, if needed, further testing.
- What are the most common acid reflux causes?
The most common causes are a weakened lower esophageal sphincter, hiatal hernia, obesity, eating large meals or eating late at night, smoking, pregnancy, and certain medications. Dietary triggers like alcohol, caffeine, and fatty foods worsen reflux but are often contributing factors rather than root causes.
- Can persistent heartburn cause cancer?
Chronic, untreated GERD can lead to Barrett’s esophagus — a change in the esophageal lining — which carries a small but elevated risk of esophageal adenocarcinoma. This is why persistent heartburn that doesn’t respond to standard treatment should be evaluated with an endoscopy.
- Are PPIs safe for long-term use?
PPIs are effective and generally safe for short-to-medium term use. Long-term use without reassessment has associations with magnesium deficiency, potential effects on bone density, and kidney health. They shouldn’t be taken indefinitely without periodic review with your doctor to assess whether they remain necessary.
- Does stress cause heartburn?
Stress doesn’t directly cause acid reflux physiologically, but it amplifies perception of symptoms and can worsen GI motility. Many people also eat differently, sleep less, and drink more alcohol during stressful periods — all of which contribute to reflux. The connection is real even if it’s partly indirect.







