A Screening Test Nobody Wants — And Why That Doesn’t Matter
Let’s be honest about this. However, doctors strongly recommend colonoscopy after age 45 because it helps detect colorectal cancer at an early stage.
. The prep is unpleasant. The idea of sedation makes some people anxious. The whole thing requires a day out of your schedule, someone to drive you home, and a degree of vulnerability that most people would prefer to avoid. So the fact that doctors continue to recommend it — firmly, consistently, with some urgency — is worth paying attention to. They’re not recommending it because it’s convenient. They’re recommending it because it works.

And now the recommendation has moved. Used to be 50 was the age where colonoscopy after age 45 was discussed. The American Cancer Society updated their guidelines in 2018, and several other major health organizations followed. The new threshold is 45. That change didn’t happen arbitrarily.
Colonoscopy after age 45 is recommended because colorectal cancer rates are increasing in younger adults. The procedure allows doctors to detect and remove precancerous polyps early, significantly reducing the risk of colon cancer.
Why Colonoscopy After Age 45 Is Now Recommended
The growing evidence of cancer cases in younger adults is one reason colonoscopy after age 45 has become a standard screening recommendation.
The data showed something unsettling. Cases of colorectal cancer in adults under 50 have been rising steadily for about three decades. The overall colorectal cancer incidence in older adults has declined — largely because of screening. More colonoscopies, more polyps caught, more cancers prevented. But in the under-50 age group, rates have been going up.
This is what epidemiologists call an ’emerging trend.’ It doesn’t mean young people are suddenly getting colorectal cancer at alarming rates overall. It means the historical assumption that colon cancer is primarily an older person’s disease needs adjusting. The biology of the colon doesn’t wait until your 50th birthday to start behaving differently.
Moving preventive colonoscopy to age 45 for average-risk adults gives a wider window to catch changes before they become serious. The math on that — catching precancerous polyps at 47 versus finding a cancer at 53 — is not subtle.
What Happens During a Colonoscopy After Age 45
A colonoscopy after age 45 allows doctors to detect and remove precancerous polyps before they develop into cancer.
A colonoscopy benefits discussion has to start with what the procedure actually involves. A flexible scope with a camera is guided through the entire length of the large intestine. The gastroenterologist or colorectal surgeon looks directly at the lining of the colon for any abnormalities.
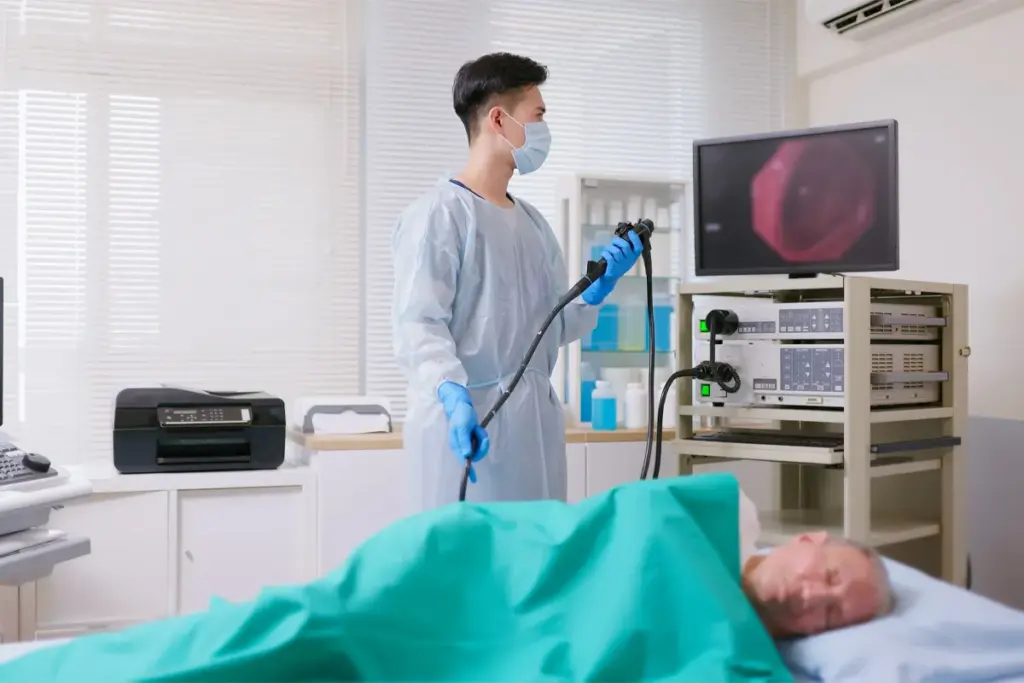
Polyps — small growths on the colon wall — are the main thing being looked for. Most polyps are benign. Some are precancerous. A small percentage are already malignant. The critical window is that precancerous stage. Polyps can be removed during the colonoscopy itself, in the same procedure. That’s not nothing. That’s the cancer that doesn’t happen.
Other things a colonoscopy can identify:
- Inflammation (suggesting IBD, colitis, Crohn’s disease)
- Diverticulosis — small pouches in the colon wall
- Bleeding sources that aren’t explained by other means
- Early-stage colorectal cancer that is completely asymptomatic
Colon Cancer Screening — The Broader Picture
Among all screening options, colonoscopy after age 45 remains one of the most effective methods for preventing colorectal cancer.
colonoscopy after age 45 is one option within colon cancer screening, not the only one. Other methods exist — stool DNA tests, FIT tests (fecal immunochemical tests), CT colonography. Each has different sensitivity, specificity, cost implications, and follow-up requirements.
What distinguishes the colonoscopy from the others is that it is both diagnostic and therapeutic in a single procedure. If a stool test comes back positive, the next step is a colonoscopy anyway. If CT colonography finds a polyp, a colonoscopy follows. The colonoscopy is often the endpoint regardless.
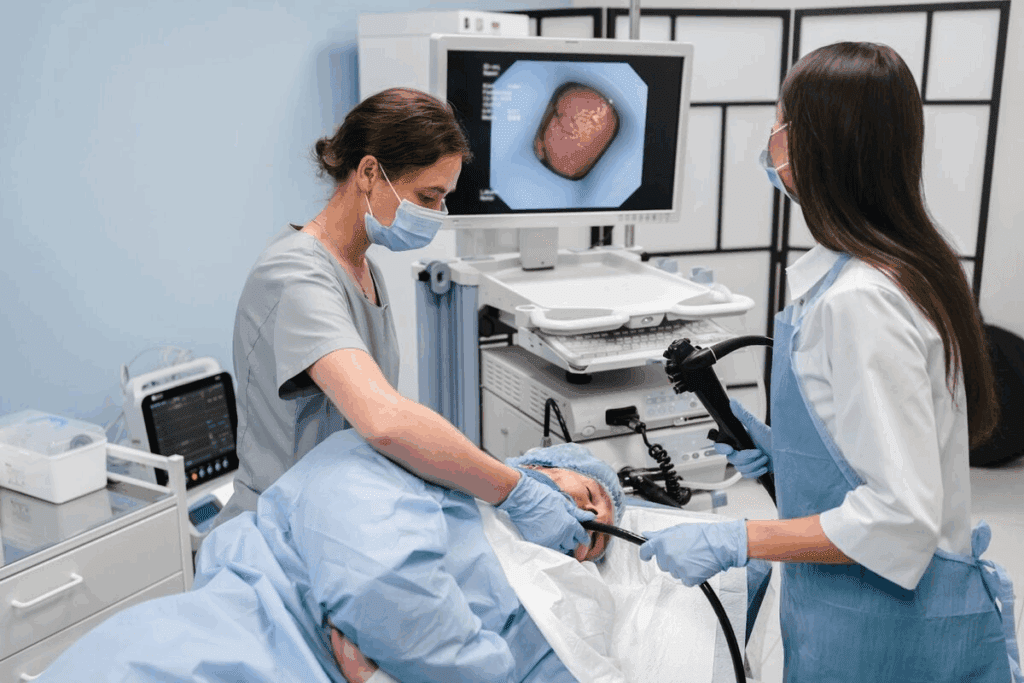
For average-risk individuals, a colonoscopy every ten years starting at 45 is a common recommendation. If polyps are found, the follow-up interval may be shorter — three to five years depending on size, type, and number. High-risk individuals — those with a family history of colorectal cancer, certain hereditary syndromes, or a personal history of IBD — may start screening earlier and more frequently.
Among all screening options, colonoscopy remains the most reliable method for detecting colon abnormalities early. Understanding the full importance of colonoscopy for early detection and prevention can help patients make informed screening decisions.
What ‘Average Risk’ and ‘High Risk’ Actually Mean
Average risk means you don’t have specific factors that would elevate your probability above the general population baseline. No family history of colorectal cancer or polyps in a first-degree relative under 60. No personal history of colorectal cancer, IBD, or certain hereditary syndromes like Lynch syndrome or familial adenomatous polyposis.
If any of those apply to you, guidelines typically recommend starting colon cancer screening earlier — sometimes as early as 25 to 40 depending on the specific condition and family history. This is something to discuss with your doctor, not self-determine.
Risk factors that can influence colon health include:
- Diet high in processed meats and low in fiber
- Obesity, particularly central obesity
- Heavy alcohol use
- Smoking
- Physical inactivity
- Type 2 diabetes
None of these make a colonoscopy more immediately urgent at 40 versus 45 for average-risk individuals, but they’re part of the conversation your doctor should be having with you.
Digestive symptoms such as abdominal discomfort, irregular bowel habits, or chronic bloating after meals may sometimes signal underlying gastrointestinal conditions that require medical evaluation..
The Preparation — Honestly
The prep is the part that keeps people from scheduling. It involves a bowel cleanse the day before — a combination of dietary restriction and a laxative solution that clears the colon completely. It is not a pleasant day. It’s inconvenient, it requires staying home, and the solution itself is not exactly enjoyable to drink.
But. The cleanse is what makes the procedure accurate. An inadequately prepped colon means polyps can be hidden behind residue, which means they can be missed, which means the whole point of the screening is compromised. Modern prep formulas are better than they used to be — lower volume, better tolerated. Some gastroenterology practices now offer split-dose preps where half is taken the night before and half the morning of the procedure, which many people find more manageable.
The procedure itself is typically done under conscious sedation (sometimes called ‘twilight sedation’). Most people remember nothing. It takes roughly 30 to 60 minutes. You’re observed briefly afterward, then go home. The main restriction is not driving the day of the procedure due to the sedation.
Benefits of Getting a Colonoscopy After Age 45
Colorectal cancer is the third most commonly diagnosed cancer in the United States. It’s also one of the most preventable. The polyp-to-cancer progression typically takes years — often ten or more. That time gap is the opportunity. A colonoscopy after age 45 that finds a precancerous polyp and removes it doesn’t just identify a risk — it eliminates it.
The screening colonoscopy is one of the clearest examples of a test that reduces cancer mortality in a measurable, documented way. The evidence isn’t contested. The debate isn’t about whether it works. The challenge is getting people to actually do it.
There’s also the consideration of peace of mind. A clean colonoscopy after age 45 means you can largely set aside worry about colorectal cancer for a decade. That’s a decade of not having that background anxiety. For people with a family history who’ve been thinking about it for years, that clearance carries real weight.
What to Expect After the Procedure
The colonoscopy results are usually communicated the same day, while you’re recovering. If polyps were removed, they’ll be sent to pathology and you’ll typically get results within a week or two. Your gastroenterologist will let you know what was found, what was removed, and when your next screening should be scheduled.
Mild bloating and gas after the procedure is completely normal — the colon is inflated with air during the exam to improve visibility, and that takes a little while to pass. Most people eat normally that evening. Return to regular activity is typically the following day.
Serious complications from colonoscopy are rare — perforation occurs in roughly 1 in 1000 procedures, and post-polypectomy bleeding in approximately 1 in 200 to 1 in 500. These numbers need to be weighed against the risk of undetected colorectal cancer. For most people, that weighing isn’t close.
Conclusion
Getting a colonoscopy after age 45 can significantly reduce the risk of colorectal cancer by detecting and removing precancerous polyps early.
The move to recommend colonoscopy after age 45 reflects a genuine shift in the data — younger adults are increasingly affected by colorectal cancer, and the screening window needed to move earlier to keep up. The procedure remains the most effective tool available for colon cancer screening: direct visualization, same-session treatment of polyps, ten years of meaningful protection if the result is clean.
Nobody enjoys scheduling it. The prep is what it is. But colorectal cancer found at stage one has a roughly 90% five-year survival rate. Found at stage four, that drops below 15%. The screening doesn’t guarantee anything. But it changes the odds substantially. That’s what preventive medicine is supposed to do.

Frequently Asked Questions
- At what age should I get my first colonoscopy?
For average-risk adults, current guidelines recommend starting at age 45. If you have a family history of colorectal cancer or polyps in a first-degree relative under 60, or a personal history of IBD or hereditary syndromes, you may need to start earlier — discuss the specific timeline with your gastroenterologist.
- How often do I need a colonoscopy?
For average-risk individuals with a normal result, every 10 years is the standard recommendation. If polyps are found and removed, the interval is typically shortened to 3 or 5 years depending on the size, type, and number of polyps.
- Is colonoscopy the only option for colon cancer screening?
No. Options include annual FIT tests (fecal immunochemical tests), stool DNA tests (like Cologuard) every 1 to 3 years, and CT colonography every 5 years. However, a positive result on any of these requires a follow-up colonoscopy. Many guidelines still favor colonoscopy as the primary method because it combines detection and treatment in one procedure.
- What are the benefits of colonoscopy compared to other screening methods?
The primary colonoscopy benefit is that polyps can be removed during the same procedure — no second visit, no separate intervention. It also provides direct visualization of the entire colon, which is more thorough than indirect methods. The tradeoff is the prep, the sedation, and the need for someone to drive you home.
- Is colonoscopy dangerous?
Serious complications are rare. The risks include perforation (approximately 1 in 1000), post-polypectomy bleeding (approximately 1 in 200 to 500), and reactions to sedation. For the vast majority of people, the risk of the screening procedure is substantially lower than the risk of undetected colorectal cancer. Your doctor will go through your specific health situation before the procedure.







